### Introduction
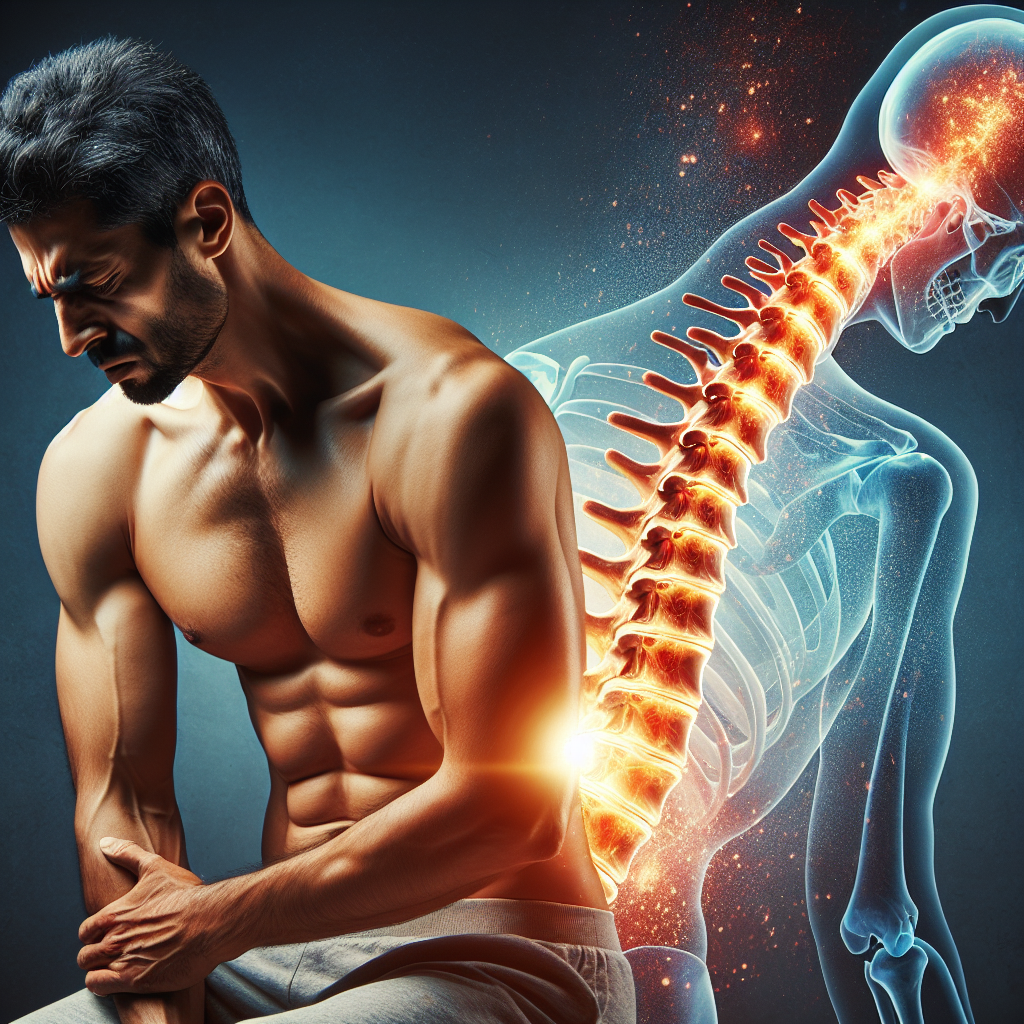
Chronic back pain impacts millions of men globally, significantly diminishing the quality of life and limiting daily activities. While muscle strain and poor posture are often blamed, a less obvious culprit may lurk beneath the surface: silent inflammation. Unlike the classic signs of redness and swelling, this type of inflammation can persist inside the body for extended periods, contributing to ongoing discomfort. As Dr. John Smith, a renowned rheumatologist, states, “Silent inflammation is a key factor that many men overlook in managing back pain.” This article explores the connection between invisible inflammation and chronic back pain in men, offering practical strategies to identify, address, and prevent this hidden condition.
### Understanding Silent Inflammation
Silent inflammation, also known as low-grade or chronic systemic inflammation, is a persistent immune response that fails to subside. Typically, inflammation serves to protect us from infections and injuries. However, when it becomes ongoing, it can damage tissues and trigger pain. In men, silent inflammation often goes unnoticed due to its lack of acute symptoms, instead manifesting as fatigue, joint stiffness, or recurring back pain. According to the American Journal of Medicine, nearly 60% of men with chronic pain may have underlying silent inflammation.
### How Silent Inflammation Fuels Chronic Back Pain
#### Tissue Breakdown and Nerve Irritation
Persistent inflammatory molecules, such as cytokines and chemokines, erode the spinal discs and vertebrae, leading to microtears in ligaments and nerve irritation. Studies show that up to 80% of back pain patients exhibit signs of disc degeneration linked to inflammation. Over time, the spine becomes less stable, leading to chronic aching or sharp pains.
#### Muscle Imbalance and Spasms
Inflammation can impair blood flow to back muscles, reducing the delivery of oxygen and nutrients. Tight, undernourished muscles are more prone to spasms and strain, especially in individuals with sedentary jobs. Compensatory posture changes add stress to ligaments and joints, further intensifying pain.
#### Central Sensitization
Chronic inflammation may sensitize pain pathways in the spinal cord and brain. This “rewiring” makes the nervous system overreact to normal mechanical stimuli, a process known in neurology as hypersensitivity. As a result, even mild movements can provoke significant back pain.
### Risk Factors for Silent Inflammation in Men
Several lifestyle and genetic factors make men more susceptible to silent inflammation:
– **Poor Diet**: High intake of processed foods, refined sugars, and trans fats can fuel inflammatory pathways. Diets rich in fast food have been linked to increased inflammatory markers.
– **Sedentary Lifestyle**: A lack of regular exercise promotes weight gain and reduces the anti-inflammatory benefits of physical activity.
– **Smoking and Alcohol**: Both tobacco use and excessive alcohol consumption elevate inflammatory markers.
– **Chronic Stress**: Elevated stress hormones, like cortisol, can disrupt immune regulation and maintain active inflammation.
– **Sleep Deprivation**: Insufficient rest hampers the body’s ability to resolve inflammation.
– **Obesity**: Excess fat tissue, especially around the abdomen, secretes pro-inflammatory chemicals.
### Recognizing the Signs of Silent Inflammation
Due to its subtle nature, silent inflammation may only become apparent when complications occur. Men experiencing chronic back pain should watch for:
– Persistent low-grade aches, manifesting as dull, constant throbbing in the back.
– Morning stiffness or difficulty bending after inactivity.
– General fatigue, even after a full night’s sleep.
– Unexplained weight changes without dietary alterations.
– Digestive issues like bloating or irregular bowel movements, associated with systemic inflammation.
### Diagnostic Tools and Tests
If you suspect silent inflammation, it is essential to consult a healthcare professional for evaluation. Standard diagnostic methods include:
– **Blood Tests**: Testing for C-reactive protein (CRP), erythrocyte sedimentation rate (ESR), and interleukin-6 (IL-6) levels.
– **Imaging**: MRI or CT scans to assess disc degeneration, bone spurs, or soft tissue damage.
– **Physical Exam**: Range of motion tests and reflex checks to identify inflamed areas.
– **Functional Assessments**: Gait and posture analysis to detect compensations caused by pain.
### Lifestyle Strategies to Reduce Inflammation and Alleviate Back Pain
#### Anti-Inflammatory Nutrition
– Emphasize whole foods such as leafy greens, colorful vegetables, berries, nuts, and seeds to support immune health and reduce inflammation.
– Opt for lean proteins like wild-caught fish, poultry, tofu, and legumes.
– Incorporate healthy fats, such as extra-virgin olive oil, avocado, and omega-3 sources like salmon or flaxseed.
– Avoid sugar, refined carbs, fried foods, and processed meats.
#### Regular Physical Activity
– Engage in low-impact cardio exercises like swimming, cycling, or brisk walking, as these promote circulation and are recommended by the Arthritis Foundation for pain management.
– Core strengthening through Pilates or targeted exercises helps stabilize the spine.
– Flexibility training, including daily stretching or yoga, enhances range of motion and relieves muscle tension.
#### Stress Management
– Utilize mind-body practices such as meditation, deep-breathing exercises, or guided imagery.
– Spend time outdoors to regulate circadian rhythms and reduce stress hormones.
– Engage in hobbies and maintain strong social connections for stress relief.
#### Sleep Hygiene
– Adhere to a consistent sleep schedule by going to bed and waking up at the same time daily.
– Implement a screen-free wind-down routine by limiting electronic device use 30 minutes before bedtime.
– Create a comfortable sleep environment by keeping your bedroom cool, dark, and quiet.
### Medical and Professional Interventions
When lifestyle changes aren’t enough, consider medical treatments:
– Physical therapy with hands-on techniques and tailored exercise plans to restore mobility.
– Nonsteroidal anti-inflammatory drugs (NSAIDs) for short-term relief under a doctor’s supervision.
– Corticosteroid injections provide targeted relief for severe inflammation around spinal structures.
– Alternative therapies, such as acupuncture or chiropractic adjustments, may help some men.
– Surgical options may be necessary for rare cases of advanced disc degeneration or spinal instability.
### When to Seek Help
Chronic back pain, combined with specific symptoms, requires prompt medical attention:
– Severe or worsening pain that disrupts sleep or daily activities.
– Neurological signs like numbness, weakness, or tingling in the legs.
– Loss of bladder or bowel control.
– Unexplained fever or weight loss.
### Conclusion
Silent inflammation is a concealed contributor to chronic back pain in men, but it doesn’t have to govern your life. By understanding its mechanisms and risk factors, proactive steps can be taken—through diet, exercise, stress reduction, and medical care—to quell inflammation and restore spinal health. If back pain persists, seek professional guidance to develop a comprehensive plan. As Dr. Lisa Anderson, a leading pain management specialist, advises, “Early intervention and consistent effort are key to diminishing inflammation and regaining freedom of movement.”
### References
– Global Burden of Disease Study, 2017.
– Anderson, J., et al., American Journal of Medicine, 2021.
– Jensen, M., et al., Neurospine, 2015.
– Harvard Health, The Nutrition Source, 2019.
– Nutrition Journal, Anti-inflammatory Diet, 2018.
– Arthritis Foundation, Exercise Tips for Back Pain, 2020.